Application of gastrointestinal pacing therapy in patients with chronic obstructive pulmonary disease complicated with gastrointestinal dysfunction
-
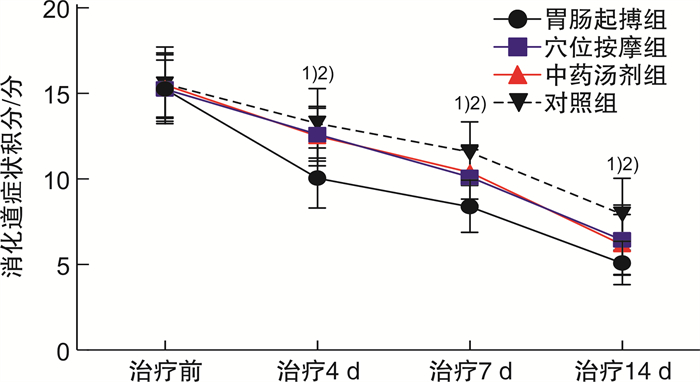
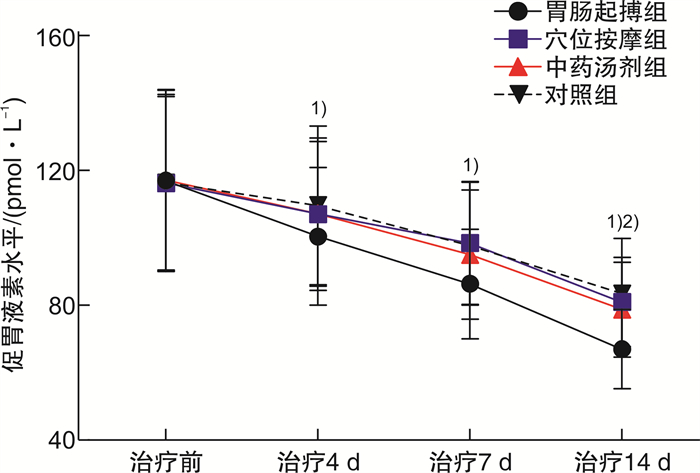
摘要: 目的 探讨胃肠起搏治疗在慢性阻塞性肺疾病(COPD)合并胃肠功能紊乱患者中的应用疗效。方法 选取2020年9月—2021年9月盐城市第三人民医院收治的COPD合并胃肠功能紊乱患者80例作为研究对象,按照随机数表法分为胃肠起搏组、中药汤剂组、穴位按摩组和对照组,每组各20例,并予以对应治疗,疗程均为14 d。分别检测4组患者治疗前后肺功能、动脉血气分析、免疫功能及促胃液素水平,记录患者治疗前后COPD评估测试量表(CAT)评分、呼吸困难指数(mMRC)评分、6分钟步行试验(6MWT)距离、生活质量(QOL)评分及消化道症状积分,并统计4组患者临床疗效。结果 胃肠起搏组患者治疗后第1秒末用力呼气量(FEV1)、第1秒末用力呼气量与用力肺活量比值(FEV1/FVC)均稍高于其他3组(P>0.05);4组患者治疗后酸碱度(pH)、血氧饱和度(SPO2)、氧分压(PO2)、二氧化碳分压(PCO2)均差异无统计学意义(P>0.05);胃肠起搏组患者治疗后CD3+、CD4+均明显高于其他3组(P< 0.05),CD8+明显低于其他3组(P< 0.05);胃肠起搏组患者治疗14 d后促胃液素水平均明显低于其他3组(P< 0.05);胃肠起搏组患者治疗后CAT及mMRC评分均明显低于其他3组(P< 0.05);胃肠起搏组患者治疗后6MWT距离明显长于其他3组(P< 0.05),QOL评分明显低于其他3组(P< 0.05);胃肠起搏组患者治疗4、7、14 d后消化道积分均明显低于其他3组(P< 0.05);4组患者间临床疗效比较,胃肠起搏组稍高于其他3组(P>0.05)。结论 胃肠起搏治疗能有效缓解COPD合并胃肠功能紊乱患者胃肠道症状,提高患者运动耐力及免疫力,且可在一定程度上改善患者肺功能。Abstract: Objective To explore the efficacy of gastrointestinal pacing treatment in patients with chronic obstructive pulmonary disease(COPD) combined with gastrointestinal dysfunction.Methods A total of 80 patients with COPD and gastrointestinal dysfunction admitted from September 2020 to September 2021 were selected as the study subjects. They were divided into gastrointestinal pacing group, TCM decoction group, acupuncture massage group and control group, with 20 cases in each group. The corresponding treatment was given, and the course was 14 days. Lung function, arterial blood gas analysis, immune function and gastrin levels were examined before and after treatment in the four groups. The COPD assessment test scale(CAT) score, respiratory difficulty index(mMRC) score, 6-minute walk trial(6MWT) distance, quality of life(QOL) score, and digestive tract symptoms score were recorded before and after treatment in the four groups. The clinical effects of the four groups of patients were also counted.Results After treatment, forced expiratory volume at the end of the first second(FEV1), ratio of forced expiratory volume to forced vital capacity at the end of first second(FEV1/FVC) in the gastrointestinal pacing group were slightly higher than the other three groups(P>0.05); There were no significant differences in acid(pH), blood oxygen saturation(SPO2), oxygen pressure(PO2) and carbon dioxide pressure(PCO2) in the four groups, respectively(P>0.05); Patients in the gastrointestinal pacing group had significantly higher CD3+and CD4+compared with the other three groups(P< 0.05) and CD8+was significantly lower than the other three groups(P< 0.05); Patients in the gastrointestinal pacing group had significantly lower gastrin levels after 14 d than in the other three groups(P< 0.05); Both the CAT and mMRC scores were significantly lower than those in the other three groups(P< 0.05); The 6MWT distance in the gastrointestinal pacing group was significantly longer than the other three groups(P< 0.05); The QOL score was significantly lower than that in the other three groups(P< 0.05); Patients in the gastrointestinal pacing group had significantly lower GI integration after 4 d, 7 d, 14 d than the other three groups(P< 0.05); Comparison of clinical efficacy between the four groups, the gastrointestinal pacing group was slightly higher than the other three groups(P>0.05).Conclusion Gastrointestinal pacing treatment can effectively relieve gastrointestinal symptoms in patients with COPD combined with gastrointestinal dysfunction, improve patients' exercise endurance and immunity, and can improve the patient's lung function to some extent.
-

-
表 1 4组患者治疗前后肺功能指标比较
X±S 指标 胃肠起搏组
(n=20)穴位按摩组
(n=20)中药汤剂组
(n=20)对照组
(n=20)F P FEV1/L 治疗前 1.54±0.31 1.52±0.36 1.55±0.34 1.52±0.33 6.768 0.934 治疗后 1.74±0.40 1.67±0.38 1.68±0.33 1.59±0.37 9.335 0.416 FEV1/FVC/% 治疗前 52.15±10.62 52.21±10.45 52.43±10.73 52.13±9.78 7.346 0.885 治疗后 58.91±11.15 56.85±10.85 55.95±10.91 54.85±10.61 10.215 0.337 表 2 4组患者治疗前后动脉血气分析指标比较
X±S 指标 胃肠起搏组
(n=20)穴位按摩组
(n=20)中药汤剂组
(n=20)对照组
(n=20)F P pH 治疗前 7.33±0.06 7.35±0.04 7.36±0.06 7.36±0.05 0.249 0.967 治疗后 7.40±0.03 7.39±0.05 7.39±0.04 7.38±0.04 0.865 0.910 SPO2/% 治疗前 92.38±4.61 91.28±5.23 91.94±4.87 92.01±4.37 1.013 0.906 治疗后 96.48±2.091) 96.54±1.771) 95.69±2.031) 96.20±2.211) 1.034 0.818 PO2/kPa 治疗前 10.25±1.87 10.53±1.77 10.24±1.85 10.92±2.07 1.125 0.875 治疗后 11.27±1.85 11.51±2.13 11.13±1.65 11.11±1.03 1.561 0.845 PCO2/kPa 治疗前 7.88±1.91 7.69±1.85 7.50±1.94 7.49±2.01 1.432 0.863 治疗后 6.73±1.87 6.63±1.71 6.43±1.75 7.21±2.05 1.659 0.421 与同组治疗前比较,1)P < 0.05。 表 3 4组患者治疗前后免疫功能比较
%,X±S 指标 胃肠起搏组
(n=20)穴位按摩组
(n=20)中药汤剂组
(n=20)对照组
(n=20)F P CD3+ 治疗前 52.57±6.17 52.94±6.23 52.25±6.21 52.40±6.13 0.636 0.915 治疗后 61.48±7.851) 57.34±7.111) 57.56±7.261) 55.39±6.961) 4.694 0.011 CD4+ 治疗前 28.88±5.77 29.07±5.85 28.32±5.73 28.42±5.81 1.312 0.871 治疗后 37.73±6.121) 32.33±6.031) 32.97±5.871) 31.42±5.941) 5.653 < 0.001 CD8+ 治疗前 35.25±5.41 35.22±5.36 35.31±5.39 35.23±5.32 1.266 0.895 治疗后 22.52±3.331) 25.41±3.611) 25.26±3.851) 28.35±3.791) 5.967 < 0.001 与同组治疗前比较,1)P < 0.05。 表 4 4组患者治疗前后CAT及mMRC评分比较
分,X±S 指标 胃肠起搏组
(n=20)穴位按摩组
(n=20)中药汤剂组
(n=20)对照组
(n=20)F P CAT评分 治疗前 30.69±4.11 30.60±4.23 30.70±4.15 30.55±4.07 0.815 0.803 治疗后 24.85±3.611) 27.19±3.521) 27.10±3.571) 28.10±3.351) 4.329 0.018 mMRC评分 治疗前 2.85±0.81 2.85±0.76 2.90±0.79 2.80±0.77 0.893 0.772 治疗后 1.75±0.431) 2.25±0.551) 2.30±0.611) 2.35±0.641) 5.135 0.007 与同组治疗前比较,1)P < 0.05。 表 5 4组患者治疗前后6MWT距离及QOL评分比较
X±S 指标 胃肠起搏组
(n=20)穴位按摩组
(n=20)中药汤剂组
(n=20)对照组
(n=20)F P 6MWT距离/m 治疗前 250.95±31.27 252.75±33.67 248.20±32.15 250.85±32.31 0.245 0.707 治疗后 286.45±35.341) 269.80±34.711) 273.90±34.151) 262.05±33.961) 3.652 0.024 QOL评分/分 治疗前 94.55±10.25 94.50±9.96 94.70±10.12 94.60±10.08 0.353 0.632 治疗后 71.05±8.131) 81.80±8.691) 81.40±8.731) 86.05±9.161) 6.125 < 0.001 与同组治疗前比较,1)P < 0.05。 表 6 4组患者临床疗效比较
例(%) 组别 例数 显效 有效 无效 总有效 胃肠起搏组 20 9(45.00) 9(45.00) 2(10.00) 18(90.00) 穴位按摩组 20 3(15.00) 11(55.00) 6(30.00) 14(70.00) 中药汤剂组 20 6(30.00) 10(50.00) 4(20.00) 16(80.00) 对照组 20 1(5.00) 11(55.00) 8(40.00) 12(60.00) χ2 5.333 P 0.149 -
[1] Gordon A, Young M, Bihler E, et al. COPD Maintenance Pharmacotherapy[J]. Crit Care Nurs Q, 2021, 44(1): 19-25. doi: 10.1097/CNQ.0000000000000336
[2] 周雯敏, 郭乔如, 王会, 等. 慢性阻塞性肺疾病转化为肺癌的研究进展[J]. 药学学报, 2020, 55(7): 1410-1418. https://www.cnki.com.cn/Article/CJFDTOTAL-YXXB202007008.htm
[3] 焦莉, 周淼. 慢性阻塞性肺疾病合并反复性肠梗阻临证经验[J]. 中医研究, 2019, 32(5): 54-57. https://www.cnki.com.cn/Article/CJFDTOTAL-ZYYJ201905025.htm
[4] Chan KY, Li X, Chen W, et al. Prevalence of chronic obstructive pulmonary disease(COPD)in China in 1990 and 2010[J]. J Glob Health, 2017, 7(2): 020704. doi: 10.7189/jogh.07.020704
[5] 何帅, 王妍. 香砂六君子汤加味联合消化内镜治疗非静脉曲张性上消化道出血及对胃肠功能紊乱的影响[J]. 中国中西医结合消化杂志, 2020, 28(3): 219-222. http://zxpw.cbpt.cnki.net/WKD2/WebPublication/paperDigest.aspx?paperID=708fa7a0-2778-49e4-b17e-b14608677720
[6] 冯祥兴, 曾凡鹏, 植冠光, 等. 温脾汤加味对危重症COPD患者急性胃肠损伤的影响研究[J]. 现代诊断与治疗, 2019, 30(5): 693-694. https://www.cnki.com.cn/Article/CJFDTOTAL-XDZD201905009.htm
[7] 马帅. 胃肠起搏治疗112例功能性胃肠病患者的护理方法研究[J]. 中国医药指南, 2018, 16(27): 250-251. https://www.cnki.com.cn/Article/CJFDTOTAL-YYXK201827204.htm
[8] 叶钧, 魏雪梅, 陈陵, 等. 体表胃起搏治疗顽固性胃功能性消化不良的临床效果观察[J]. 医学信息, 2018, 31(11): 8-10, 14. https://www.cnki.com.cn/Article/CJFDTOTAL-YXXX201811003.htm
[9] 肖玉兰, 齐科雷, 苏宏伟, 等. 老年胃癌患者术后住院期体外胃肠起搏治疗的康复效果评价[J]. 河北医药, 2020, 42(23): 3660-3663. doi: 10.3969/j.issn.1002-7386.2020.23.036
[10] 冯娟, 陈桂兰. 大黄外敷神阙穴联合胃肠起搏在老年功能性便秘患者中的应用[J]. 中国医药导报, 2020, 17(36): 159-162. https://www.cnki.com.cn/Article/CJFDTOTAL-YYCY202036040.htm
[11] 中华医学会呼吸病学分会慢性阻塞性肺疾病学组, 中国医师协会呼吸医师分会慢性阻塞性肺疾病工作委员会. 慢性阻塞性肺疾病诊治指南(2021年修订版)[J]. 中华结核和呼吸杂志, 2021, 44(3): 170-205. https://www.cnki.com.cn/Article/CJFDTOTAL-QKYX202129002.htm
[12] 韩芳朵, 李碧珍, 吴恋恋, 等. 呼吸康复护理干预对慢性阻塞性肺疾病急性加重期患者运动耐力及呼吸困难指数的影响[J]. 中国药物与临床, 2021, 21(13): 2402-2403. https://www.cnki.com.cn/Article/CJFDTOTAL-YWLC202113092.htm
[13] 杨露露, 曲木诗玮, 司徒炫明, 等. 慢性阻塞性肺疾病稳定期患者六分钟步行试验诱导的运动性低氧的预测方法研究[J]. 中国全科医学, 2022, 25(2): 212-216. https://www.cnki.com.cn/Article/CJFDTOTAL-QKYX202202011.htm
[14] 薛佩妮, 冯敏娟, 王惠琴. 噻托溴铵粉联合糖皮质激素治疗慢性阻塞性肺疾病疗效及对患者生活质量评分的影响[J]. 陕西医学杂志, 2020, 49(2): 216-219. https://www.cnki.com.cn/Article/CJFDTOTAL-SXYZ202002024.htm
[15] 杨改玲, 冯波. 胃肠起搏治疗胃肠功能紊乱性疾病的临床疗效观察[J]. 临床医学研究与实践, 2017, 2(24): 35-36. https://www.cnki.com.cn/Article/CJFDTOTAL-YLYS201724017.htm
[16] Zhu B, Wang Y, Ming J, et al. Disease burden of COPD in China: a systematic review[J]. Int J Chron Obstruct Pulmon Dis, 2018, 13: 1353-1364.
[17] Balasuriya GK, Mohsenipour M, Brassington K, et al. Ebselen prevents cigarette smoke-induced gastrointestinal dysfunction in mice[J]. Clin Sci(Lond), 2020, 134(22): 2943-2957.
[18] 黄伟锋, 刘明, 栗华, 等. 胃肠起搏器治疗功能性胃肠病的临床疗效分析[J]. 福建医药杂志, 2017, 39(1): 116-118. https://www.cnki.com.cn/Article/CJFDTOTAL-FJYY201701045.htm
[19] 何彦侠, 薛兵. 6MWT与COPD患者肺功能的相关性及对患者预后的预测价值[J]. 西南国防医药, 2019, 29(1): 27-30. https://www.cnki.com.cn/Article/CJFDTOTAL-XNGF201901011.htm
[20] 覃尚红, 黄东挺, 宾洋雁, 等. 胃肠起搏联合认知行为治疗老年腹泻型肠易激综合征患者的疗效及对生活质量的影响[J]. 内科, 2021, 16(4): 429-432. https://www.cnki.com.cn/Article/CJFDTOTAL-NKYT202104003.htm
-




 下载:
下载: