Correlation of non-alcoholic fatty liver disease patients of different Traditional Chinese Medicine syndrome with Th17/Treg levels in the peripheral blood
-
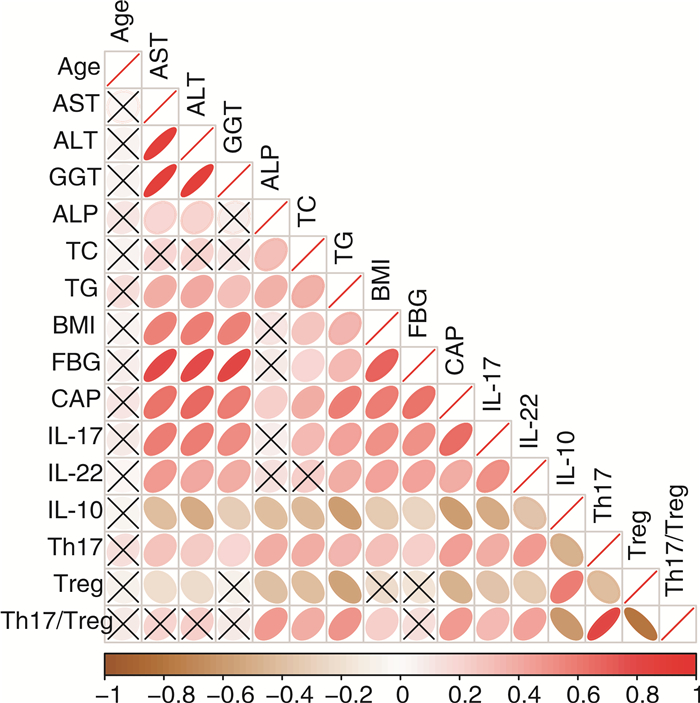
摘要: 目的 分析不同中医证型非酒精性脂肪性肝病(non-alcoholic fatty liver disease,NAFLD)与外周血辅助性T细胞17(Th17)/调节性T细胞(Treg)的相关性。方法 收集100例2022年1月—2023年4月就诊的NAFLD患者,根据中医辨证分为5个不同的中医证型组,另选取15例健康受试者作为对照组。分别检测各组受试者的肝功能、血脂、血糖、BMI、受控衰减参数(controlled attenuation parameter,CAP)值、外周血Th17/Treg和细胞因子水平,并通过Pearson检验分析病情指数与外周血T淋巴细胞水平的相关性。结果 相关性分析结果显示,NAFLD患者的丙氨酸氨基转移酶(ALT)、天门冬氨酸氨基转移酶(AST)、γ-谷氨酰基转移酶(GGT)、碱性磷酸酶(ALP)、总胆固醇(TC)、甘油三酯(TG)、BMI、空腹血糖(FBG)、CAP、IL-17、IL-22水平与Th17水平呈正相关(P<0.05),而与Treg水平呈负相关(P<0.05)。与对照组比较,NAFLD患者的AST、ALT、GGT、ALP、TC、TG、BMI、FBG、CAP、IL-17、IL-22、Th17水平和Th17/Treg比值显著升高,IL-10和Treg水平显著降低(P<0.05)。不同中医证型NAFLD患者的各项指标比较,AST、ALT、GGT、ALP、TC、TG、BMI、FBG、CAP、IL-17、IL-22、Th17水平和Th17/Treg比值按证型排序,从高到低依次为湿热蕴结证组、痰瘀互结证组、湿浊内停证组、脾肾两虚证组和肝郁脾虚证组;而不同中医证型中,Treg水平的排序则相反。结论 NAFLD患者的中医证型与Th17/Treg平衡呈现一定的相关性,其中以湿热蕴结证患者Th17水平最高。Abstract: Objective To analyze the correlation between non-alcoholic fatty liver disease(NAFLD) patients of different Traditional Chinese Medicine(TCM) syndromes with Th17/Treg in peripheral blood.Methods One hundred NAFLD patients who visited the clinic from January 2022 to April 2023 were collected and divided into five groups based on TCM syndrome, and another 15 healthy volunteers were selected as the control group. The liver function, blood lipid, blood glucose, BMI, controlled attenuation parameter(CAP) value, levels of Th17/Treg and cytokines in peripheral blood were detected respectively, and the correlation between the disease index and levels of Th17/Treg was analyzed by the Pearson test.Results The results of correlation analysis showed that the levels of liver function(ALT, AST, GGT, ALP), lipids(TC, TG), FBG, BMI, CAP, Th17/Treg, IL-17, and IL-22 in patients with NAFLD showed a significant positive correlation with Th17(P < 0.05), while a significant negative correlation was observed with Treg(P < 0.05). Compared with the control group, NAFLD patients showed significantly higher levels of liver function(ALT, AST, GGT, ALP), TC, TG, FBG, BMI, CAP, Th17, IL-17 and IL-22, and lower levels of IL-10 and Treg(P < 0.05). Comparison of various indicators in NAFLD patients with different TCM syndromes. AST, ALT, GGT, ALP, TC, TG, BMI, FBG, CAP, IL-17, IL-22, Th17 levels and Th17/Treg ratio are sorted by syndrome type. From high to low, they are the damp-heat accumulation syndrome, the phlegm stasis mutual accumulation syndrome, dampness turbidity internal cessation syndrome, spleen kidney deficiency syndrome and liver depression and spleen deficiency syndrome. However, the ranking of Treg levels showed the opposite trend in the comparison of different TCM syndromes.Conclusion There is a certain correlation between the TCM syndromes of NAFLD patients and the balance of Th17/Treg, with the highest level of Th17 in patients with the dampness heat accumulation syndrome.
-

-
表 1 受试者的临床资料比较
例,X±S 组别 例数 性别 年龄/岁 病程/年 男 女 肝郁脾虚证组 25 11 14 46.19±11.75 4.36±1.58 湿热蕴结证组 23 14 9 48.11±11.22 4.00±2.15 湿浊内停证组 17 10 7 46.77±9.51 4.06±1.82 痰瘀互结证组 22 10 12 43.51±12.89 4.91±2.30 脾肾两虚证组 13 7 6 49.09±6.76 5.69±3.04 对照组 15 8 7 41.43±5.22 表 2 各组受试者肝功能指标的比较
U/L,X±S 组别 例数 AST ALT GGT ALP 肝郁脾虚证组 25 29.68±2.782) 25.00±3.382) 38.60±3.152) 91.64±6.492) 湿热蕴结证组 23 33.48±4.111) 33.00±4.301) 42.00±4.621) 101.43±8.771) 湿浊内停证组 17 31.59±2.851) 27.59±5.271)2) 38.53±3.142) 96.00±7.882) 痰瘀互结证组 22 32.82±3.781) 29.86±6.071)2) 39.86±5.241) 98.36±9.441) 脾肾两虚证组 13 30.23±3.982) 26.46±4.162) 38.23±4.642) 93.00±5.642) 对照组 15 28.07±3.842) 24.27±5.472) 37.13±3.072) 90.93±13.672) 与对照组比较,1)P<0.05;与湿热蕴结证组比较,2)P<0.05。 表 3 各组受试者血脂、BMI和血糖水平的比较
X±S 组别 例数 TC/(mmol/L) TG/(mmol/L) BMI FBG/(mmol/L) 肝郁脾虚证组 25 5.80±0.801)2) 2.29±0.421)2) 25.12±0.771)2) 5.48±0.632) 湿热蕴结证组 23 6.38±0.761) 3.54±1.181) 26.13±1.261) 5.97±0.781) 湿浊内停证组 17 6.28±0.771) 2.76±0.531)2) 25.53±1.061) 5.64±0.751) 痰瘀互结证组 22 6.26±0.981) 3.13±0.871) 26.08±1.131) 5.80±0.651) 脾肾两虚证组 13 5.86±0.511) 2.33±0.271)2) 25.34±1.071) 5.62±0.931) 对照组 15 4.48±0.442) 1.29±0.262) 23.66±3.20 5.05±0.572) 与对照组比较,1)P<0.05;与湿热蕴结证组比较,2)P<0.05。 表 4 各组受试者炎症因子水平的比较
ng/L,X±S 组别 例数 IL-17 IL-22 IL-10 肝郁脾虚证组 25 38.76±10.161)2) 37.39±11.432) 14.28±1.882) 湿热蕴结证组 23 49.78±10.841) 45.80±8.911) 8.60±1.041) 湿浊内停证组 17 45.29±11.481) 40.47±6.561) 12.05±2.021)2) 痰瘀互结证组 22 47.83±10.571) 44.25±12.461) 10.07±1.581)2) 脾肾两虚证组 13 42.62±11.571) 39.01±9.142) 13.03±1.661)2) 对照组 15 22.00±4.052) 28.32±6.782) 15.85±2.002) 与对照组比较,1)P<0.05;与湿热蕴结证组比较,2)P<0.05。 表 5 各组受试者Th17、Treg、Th17/Treg水平的比较
X±S 组别 例数 Th17/% Treg/% Th17/Treg 肝郁脾虚证组 25 3.56±0.601)2) 4.85±0.631)2) 0.75±0.161)2) 湿热蕴结证组 23 4.62±1.181) 3.49±0.641) 1.35±0.361) 湿浊内停证组 17 3.92±0.671)2) 4.53±0.561)2) 0.87±0.151)2) 痰瘀互结证组 22 4.33±0.901) 3.95±0.931)2) 1.17±0.401)2) 脾肾两虚证组 13 3.68±0.701)2) 4.75±0.651)2) 0.79±0.181)2) 对照组 15 2.53±0.582) 6.13±1.042) 0.42±0.102) 与对照组比较,1)P<0.05;与湿热蕴结证组比较,2)P<0.05。 -
[1] Tilg H, Adolph TE, Moschen AR. Multiple Parallel Hits Hypothesis in Nonalcoholic Fatty Liver Disease: Revisited After a Decade[J]. Hepatology, 2021, 73(2): 833-842. doi: 10.1002/hep.31518
[2] Wong WK, Chan WK. Nonalcoholic Fatty Liver Disease: A Global Perspective[J]. Clin Ther, 2021, 43(3): 473-499. doi: 10.1016/j.clinthera.2021.01.007
[3] 魏芳, 范梦慧, 刘光臣, 等. 脆弱拟杆菌ATCC25285通过TGF-β/Smad3通路诱导Treg细胞分化缓解结肠炎[J]. 中国药科大学学报, 2023, 54(2): 226-237. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGYD202302011.htm
[4] Lourenco JD, Ito JT, Martins MA, et al. Th17/Treg Imbalance in Chronic Obstructive Pulmonary Disease: Clinical and Experimental Evidence[J]. Front Immunol, 2021, 12: 804919. doi: 10.3389/fimmu.2021.804919
[5] 李向阳, 高春耕, 王全智. 大黄利胆胶囊联合水飞蓟宾葡甲胺治疗非酒精性脂肪性肝病的临床研究[J]. 现代药物与临床, 2021, 36(2): 340-344. https://www.cnki.com.cn/Article/CJFDTOTAL-GWZW202102027.htm
[6] 邱晨, 杨红岩, 张倩, 等. IL-35与肝脏疾病的关系[J]. 肝脏, 2022, 38(12): 1347-1351. doi: 10.3969/j.issn.1008-1704.2022.12.025
[7] 涂晓娟, 张朝玉, 刘丹, 等. CD4+CD25+调节性T细胞通过抑制B细胞对小鼠自身免疫性卵巢疾病发挥治疗作用[J]. 免疫学杂志, 2022, 38(12): 1030-1037. https://www.cnki.com.cn/Article/CJFDTOTAL-MYXZ202212003.htm
[8] Wang X, Li W, Fu J, et al. Correlation between T-Lymphocyte Subsets, Regulatory T Cells, and Hepatic Fibrosis in Patients with Nonalcoholic Fatty Liver[J]. Evid Based Complement Alternat Med, 2022, 31(2022): 6250751.
[9] 中国中西医结合学会消化系统疾病专业委员会. 非酒精性脂肪性肝病中西医结合诊疗共识意见(2017年)[J]. 中国中西医结合消化杂志, 2017, 25(11): 805-811. https://zxyxh.whuhzzs.com/article/doi/10.3969/j.issn.1671-038X.2017.11.02
[10] 祝思思, 王炳予, 杨磊, 等. 不同中医证型非酒精性脂肪性肝炎患者肠道菌群差异性研究[J]. 中国中西医结合消化杂志, 2023, 31(10): 781-787. doi: 10.3969/j.issn.1671-038X.2023.10.10
[11] 中华医学会肝病学分会脂肪肝和酒精性肝病学组, 中国医师协会脂肪性肝病专家委员会. 非酒精性脂肪性肝病防治指南(2018更新版)[J]. 传染病信息, 2018, 31(5): 393-402, 420. https://www.cnki.com.cn/Article/CJFDTOTAL-CRBX201805002.htm
[12] 刘婧, 李燕菊, 饶志勇. 非酒精性脂肪性肝病患者FibroScan指标与人体成分指标相关性分析[J]. 中西医结合肝病杂志, 2021, 31(12): 1108-1111. https://www.cnki.com.cn/Article/CJFDTOTAL-ZXGB202112014.htm
[13] Zhu Y, Liu R, Shen Z, et al. Combination of luteolin and lycopene effectively protect against the "two-hit" in NAFLD through Sirt1/AMPK signal pathway[J]. Life Sci, 2020, 256: 117990. doi: 10.1016/j.lfs.2020.117990
[14] 廖红芳, 杨雨航. 2型糖尿病合并非酒精性脂肪肝与胰岛素抵抗的相关性[J]. 实用糖尿病杂志, 2020, 16(3): 17-18. https://www.cnki.com.cn/Article/CJFDTOTAL-LNSY202003017.htm
[15] 赵长龄, 李红良. 非酒精性脂肪性肝病的发病机制研究[J]. 华南国防医学杂志, 2020, 34(7): 525-527. https://www.cnki.com.cn/Article/CJFDTOTAL-HNGY202007019.htm
[16] 张珂瓈, 李昌平. 肠道微生物群与代谢相关性脂肪性肝病关系的研究进展[J]. 现代临床医学, 2023, 49(3): 223-225, 229. https://www.cnki.com.cn/Article/CJFDTOTAL-YYCD202303019.htm
[17] 叶子昊, 祝可欣, 贺宇涵, 等. 非酒精性脂肪肝的发病机制及潜在药物研究进展[J]. 河北医药, 2023, 45(22): 3484-3488. https://www.cnki.com.cn/Article/CJFDTOTAL-HBYZ202322027.htm
[18] 施漪雯, 范建高. 代谢相关性脂肪性肝病流行现状[J]. 实用肝脏病杂志, 2023, 26(6): 777-780. https://www.cnki.com.cn/Article/CJFDTOTAL-GBSY202306003.htm
[19] 王木源, 李军祥, 卢心毓, 等. 清肠温中方对溃疡性结肠炎小鼠组织驻留记忆CD4+T细胞的调控作用[J]. 中国中西医结合消化杂志, 2023, 31(8): 583-588. https://zxyxh.whuhzzs.com/article/doi/10.3969/j.issn.1671-038X.2023.08.02
[20] Mendez-Sanchez N, Valencia-Rodriguez A, Coronel-Castillo C, et al. The cellular pathways of liver fibrosis in non-alcoholic steatohepatitis[J]. Ann Transl Med, 2020, 8(6): 400. doi: 10.21037/atm.2020.02.184
[21] 王秋莹, 马玲. 血清Chemerin、IL-17与非酒精性脂肪性肝病的相关性研究[J]. 宁夏医学杂志, 2021, 43(4): 327-329. https://www.cnki.com.cn/Article/CJFDTOTAL-NXYX202104016.htm
[22] Chen J, Zhou H, Jin H, et al. Role of Inflammatory Factors in Mediating the Effect of Lipids on Nonalcoholic Fatty Liver Disease: A Two-Step, Multivariable Mendelian Randomization Study[J]. Nutrients, 2022, 14(20): 4434. doi: 10.3390/nu14204434
[23] 蔡春雨, 李琳, 酒晓盈, 等. 不同病理分型脑胶质瘤切除患者Th17/Treg相关细胞因子及其与术后颅内感染的关系[J]. 中华医院感染学杂志, 2023, 33(11): 1646-1649. https://www.cnki.com.cn/Article/CJFDTOTAL-ZHYY202311010.htm
[24] 唐家琢, 李满, 王卫星, 等. Treg在肝移植受者免疫耐受中的研究进展[J]. 中华肝脏外科手术学电子杂志, 2021, 10(3): 337-339. doi: 10.3877/cma.j.issn.2095-3232.2021.03.022
[25] 李瑞风, 宗廷妮, 戴光荣. IL-10对非酒精性脂肪性肝病发病的保护机制及其治疗前景[J]. 临床肝胆病杂志, 2022, 38(12): 2836-2840. https://www.cnki.com.cn/Article/CJFDTOTAL-LCGD202212025.htm
[26] 张圣江, 周杨, 柯淑红, 等. 五苓散加味联合水飞蓟宾对痰瘀互结型非酒精性脂肪性肝病患者肝功能、血脂和Th17/Treg平衡状态的影响[J]. 中西医结合肝病杂志, 2021, 31(8): 691-694. https://www.cnki.com.cn/Article/CJFDTOTAL-ZXGB202108007.htm
[27] Li Y, Gao S, Shi S, et al. Tetrahedral Framework Nucleic Acid-Based Delivery of Resveratrol Alleviates Insulin Resistance: From Innate to Adaptive Immunity[J]. Nanomicro Lett, 2021, 13(1): 86.
[28] Asadi-Samani M, Bagheri N, Rafieian-Kopaei M, et al. Inhibition of Th1 and Th17 Cells by Medicinal Plants and Their Derivatives: A Systematic Review[J]. Phytother Res, 2017, 31(8): 1128-1139. doi: 10.1002/ptr.5837
[29] Nian F, Wu L, Xia Q, et al. Akkermansia muciniphila and Bifidobacterium bifidum Prevent NAFLD by Regulating FXR Expression and Gut Microbiota[J]. J Clin Transl Hepatol, 2023, 11(4): 763-776.
-

计量
- 文章访问数: 230
- 施引文献: 0



 下载:
下载: