Effect of HBV infection on liver metastasis of pancreatic cancer patients after radical operation
-
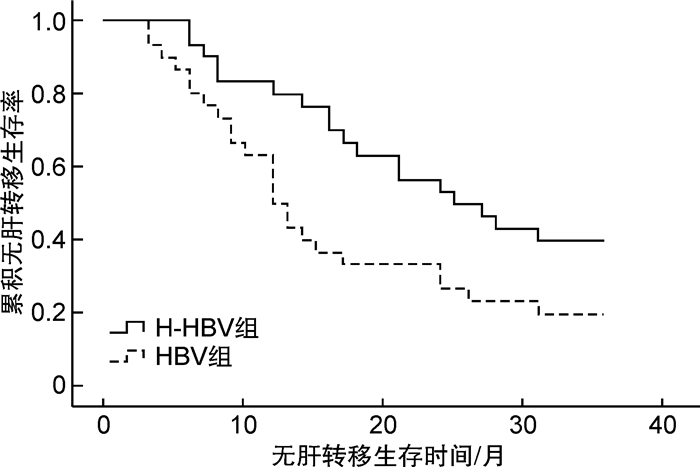
摘要: 目的 探讨乙肝病毒(HBV)感染对胰腺癌患者根治术后肝转移的影响。方法 回顾性分析2013年1月—2015年12月接受胰腺癌根治术的156例患者的临床病理资料,采用Kaplan-Meier单因素分析比较各临床病理因素分组胰腺癌术后无肝转移生存率、Cox单因素和多因素分析获得影响胰腺癌患者根治术后肝转移的独立预测因素,Kaplan-Meier生存分析比较HBV和N-HBV2组患者胰腺癌术后无肝转移生存率。结果 156例接受胰腺癌根治术患者,其中男105例(67.3%),女51例(32.7%),平均年龄为(53.8±10.9)岁,胰腺癌根治术后1年、2年、3年肝转移发生率分别为33.5%、48.9%和56.3%,Cox多因素分析结果显示,TNM/T分期、血管神经侵犯、HBV感染以及HBV-DNA为影响胰腺癌患者根治术后肝转移的独立预测因素,其中TNM/T2+T3分期胰腺癌术后肝转移的风险是TNM/T1分期的4.654倍(HR:4.654,95%CI:3.876~5.432,P=0.000),伴有血管神经侵犯患者胰腺癌术后肝转移的风险是无血管神经侵犯的4.215倍(HR:4.215,95%CI:3.245~5.125,P=0.011),HBV感染患者胰腺癌术后肝转移的风险是非HBV感染患者的2.817倍(HR:2.817,95%CI:2.135~3.568,P=0.026),Kaplan-Meier生存分析显示,N-HBV组胰腺癌术后1年、2年、3年的无肝转移生存率明显高于HBV组(73.6%、57.4%、43.1% vs. 61.5%、38.4%、30.4%,P< 0.05)。结论 胰腺癌术后肝转移与TNM/T分期、肿瘤血管神经侵犯及伴有HBV感染密切相关。Abstract: Objective To investigate the effect of HBV infection on liver metastasis of pancreatic cancer patients after radical operation.Methods The clinicopathological data of 156 patients with pancreatic cancer who underwent radical surgery from January 2013 to December 2015 were retrospectively analyzed. Kaplan-Meier univariate analysis was used to compare the liver metastasis free survival rate of post operative pancreatic cancer patients between different clinicopathological factor group. Cox univariate analysis and multivariate analysis were used to obtain independent predictors of infecting liver metastasis of pancreatic cancer patients after radical surgery, Kaplan-Meier survival analysis was used to compare the liver metastasis free survival rates of postoperative patients between HBV infection and N-HBV infection.Results 156 patients with pancreatic cancer underwent radical operation, the average age was (53.8±10.9), among them, 105(67.3%) were male and 51(32.7%) were female. The 1-year, 2-year, and 3-year liver metastasis rates were 33.5%, 48.9%, and 56.3%, respectively. The results of Cox multivariate analysis showed that TNM / T stage, vascular nerve invasion and HBV infection were independent predictors of infecting postoperative liver metastasis of pancreatic cancer patients. The risk of postoperative liver metastasis in TNM / T2 + T3 stage was 4.654 times higher than that in TNM / T1 stage(HR: 4.654, 95%CI: 3.876-5.432,P=0.000), the risk of postoperative liver metastasis in patients with vascular and nerve invasion was 4.215 times higher than that in patients without vascular and nerve invasion(HR: 4.215, 95%CI: 3.245-5.125,P=0.011). The risk of postoperative liver metastasis in patients with HBV infection was 2.817 times higher than that in patients without HBV infection(HR: 2.817, 95%CI: 2.135-3.568,P=0.026). Kaplan-Meier survival analysis showed that the 1-year, 2-year, 3-year liver metastasis free survival rate of postoperative N-HBV infection group was significantly higher than that in HBV infection group(73.6%, 57.4%, 43.1% vs. 61.5%, 38.4%, 30.4%,P< 0.05).Conclusion Postoperative liver metastasis of pancreatic cancer is closely related to TNM / T stage, tumor vascular and nerve invasion and HBV infection.
-
Key words:
- HBV infection /
- pancreatic cancer /
- radical operation /
- liver metastasis
-

-
表 1 影响胰腺癌患者根治术后肝转移的Kaplan-Meier单因素分析
临床病理特征 例数 累积无肝转移生存率/% χ2 P 1年 2年 3年 年龄/岁 3.125 0.075 ≥55 81 55.2 39.6 30.2 < 55 75 58.9 48.6 35.7 性别 2.867 0.081 男 105 53.2 48.1 29.5 女 51 61.6 52.5 34.8 CA-199 2.456 0.095 升高 90 51.7 45.6 31.2 正常 66 62.3 54.5 36.8 病灶位置 3.356 0.068 胰头 98 55.6 49.6 32.5 胰尾 58 68.9 41.6 30.1 病灶直径/cm 5.788 0.047 ≥2 110 55.9 35.7 29.1 < 2 46 68.5 57.1 43.5 TNM/T分期 11.276 <0.001 T1 38 69.8 50.1 39.5 T2+T3 118 50.2 29.8 18.1 分化程度 3.143 0.072 低分化 69 55.4 41.6 31.7 中高分化 87 63.7 49.8 37.6 血管神经侵犯 8.902 0.006 是 55 42.5 33.5 19.4 否 101 68.7 49.5 40.5 梗阻性黄疸 8.569 0.008 是 82 39.6 31.4 18.3 否 74 65.3 55.6 41.6 HBV感染 7.894 0.012 是 52 61.5 38.4 30.4 否 104 73.6 57.4 43.1 HBV-DNA 8.388 0.008 阳性 48 58.9 35.2 27.6 阴性 108 75.3 60.2 46.6 表 2 影响胰腺癌患者根治术后肝转移的Cox单因素分析
自变量 β SE HR 95%CI P 肿瘤大小 0.876 0.233 2.341 1.893~2.567 0.021 TNM/T期 2.314 0.187 5.134 4.123~6.224 <0.001 血管神经侵犯 2.019 0.315 4.125 3.092~5.235 0.004 梗阻性黄疸 1.894 0.209 3.895 3.012~4.673 0.009 HBV感染 1.213 0.345 2.769 2.196~3.684 0.015 HBV-DNA 1.345 0.338 3.245 2.019~3.897 0.004 表 3 影响胰腺癌患者根治术后肝转移的Cox多因素分析
自变量 β SE HR 95%CI P TNM/T期 1.896 0.218 4.654 3.876~5.432 <0.001 血管神经侵犯 1.723 0.186 4.215 3.245~5.125 0.011 HBV感染 1.014 0.314 2.817 2.135~3.568 0.026 HBV-DNA 1.235 0.287 3.117 2.175~3.887 0.009 -
[1] Golan T, Hammel P, Reni M, et al. Maintenance Olaparib for Germline BRCA-Mutated Metastatic Pancreatic Cancer[J]. N Engl J Med, 2019, 381(4): 317-327. doi: 10.1056/NEJMoa1903387
[2] Versteijne E, Suker M, Groothuis K, et al. Preoperative Chemoradiotherapy Versus Immediate Surgery for Resectable and Borderline Resectable Pancreatic Cancer: Results of the Dutch Randomized Phase Ⅲ PREOPANC Trial[J]. J Clin Oncol, 2020, 38(16): 1763-1773. doi: 10.1200/JCO.19.02274
[3] 郭忠聪, 文静. 立体定向放疗综合治疗联合自拟清毒活血汤治疗局部胰腺癌晚期患者的生存时间对比观察[J]. 中国中西医结合消化杂志, 2018, 26(3): 243-247. https://www.cnki.com.cn/Article/CJFDTOTAL-ZXPW201803005.htm
[4] 楼文晖, 方圆. 胰腺癌根治术的范围: 共识与争议[J]. 中国实用外科杂志, 2018, 38(2): 30-32. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGWK201802007.htm
[5] Palmer DH, Stocken DD, Hewitt H, et al. A randomized phase 2 trial of neoadjuvant chemotherapy in resectable pancreatic cancer: gemcitabine alone versus gemcitabine combined with cisplatin[J]. Ann Surg Oncol, 2007, 14(7): 2088-2096. doi: 10.1245/s10434-007-9384-x
[6] 张杰, 张景俊. FOLFIRINOX方案联合载药微球介入灌注化疗栓塞治疗胰腺癌肝转移1例[J]. 现代消化及介入诊疗, 2020, 25(11): 1552-1555. doi: 10.3969/j.issn.1672-2159.2020.11.034
[7] 李文迪, 陶连元, 王行雁, 等. 术前淋巴细胞/单核细胞比值与可切除性胰腺癌预后的相关性分析[J]. 中国微创外科杂志, 2018, 24(4): 289-293. https://www.cnki.com.cn/Article/CJFDTOTAL-ZWWK201804002.htm
[8] 欧阳华强, 潘战宇, 刘方, 等. 中药联合全身化疗和(或)动脉灌注化疗治疗胰腺癌肝转移的回顾性研究[J]. 中国中西医结合杂志, 2015, 35(6): 654-658. https://www.cnki.com.cn/Article/CJFDTOTAL-ZZXJ201506003.htm
[9] 孙文韬, 邓侠兴. 胰腺癌与乙型肝炎感染的研究进展[J]. 外科理论与实践, 2020, 25(2): 85-87. https://www.cnki.com.cn/Article/CJFDTOTAL-WKLL202002025.htm
[10] Motoi F, Kosuge T, Ueno H, et al. Randomized phase Ⅱ/Ⅲ trial of neoadjuvant chemotherapy with gemcitabine and S-1 versus upfront surgery for resectable pancreatic cancer(Prep-02/JSAP05)[J]. Jpn J Clin Oncol, 2019, 49(2): 190-194. doi: 10.1093/jjco/hyy190
[11] 闵永峰, 张弛, 张波. 113例胰腺癌根治术后复发及辅助治疗对生存期影响[J]. 中华肿瘤防治杂志, 2019, 26(8): 565-569. https://www.cnki.com.cn/Article/CJFDTOTAL-QLZL201908010.htm
[12] 中国抗癌协会胰腺癌专业委员会. 胰腺癌综合诊治指南(2018版)[J]. 中华外科杂志, 2018, 34(7): 481-494. https://www.cnki.com.cn/Article/CJFDTOTAL-LCGD201810011.htm
[13] 朱序勤, 贾淞淋, 祁洁, 等. 影响胰腺癌根治术预后的围手术期相关因素的回顾性分析[J]. 中国癌症杂志, 2019, 29(7): 521-527. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGAZ201907009.htm
[14] 赵玉沛, 崔铭, 张太平. 腹腔镜胰腺癌根治术的热点与展望[J]. 中华普外科手术学杂志(电子版), 2019, 13(4): 325-327. doi: 10.3877/cma.j.issn.1674-3946.2019.04.001
[15] 金凯舟, 罗国培, 程合, 刘辰, 虞先濬. 胰腺癌肝转移的综合治疗[J]. 肝胆外科杂志, 2019, 27(1): 16-20. https://www.cnki.com.cn/Article/CJFDTOTAL-GDWZ201901004.htm
[16] Oki E, Emi Y, Yamanaka T, et al. Randomised phase Ⅱ trial of mFOLFOX6 plus bevacizumab versus mFOLFOX6 plus cetuximab as first-line treatment for colorectal liver metastasis(ATOM trial)[J]. Br J Cancer, 2019, 121(3): 222-229. doi: 10.1038/s41416-019-0518-2
[17] 庄汉, 时志鹏, 胡鹏, 等. HBV感染与胰腺癌发病风险关系的荟萃分析[J]. 中华肝脏病杂志, 2014, 22(6): 416-419.
[18] Granieri S, Altomare M, Bruno F, et al. Surgical treatment of gastric cancer liver metastases: systematic review and meta-analysis of long-term outcomes and prognostic factors[J]. Crit Rev Oncol Hematol, 2021, 24(5): 103313.
[19] Wang X, Hu LP, Qin WT, et al. Identification of a subset of immunosuppressive P2RX1-negative neutrophils in pancreatic cancer liver metastasis[J]. Nat Commun, 2021, 12(1): 174.
[20] 阙海涛, 储建华, 曹斌. HBV与胰腺癌病理分化程度的关系研究[J]. 现代消化及介入诊疗, 2018, 23(6): 32-34. https://www.cnki.com.cn/Article/CJFDTOTAL-XDXH201806007.htm
[21] Andtbacka RH, Ross M, Puzanov I, et al. Patterns of Clinical Response with Talimogene Laherparepvec(T-VEC)in Patients with Melanoma Treated in the OPTiM Phase Ⅲ Clinical Trial[J]. Ann Surg Oncol, 2016, 23(13): 4169-4177.
[22] Ho TTB, Nasti A, Seki A, et al. Combination of gemcitabine and anti-PD-1 antibody enhances the anticancer effect of M1 macrophages and the Th1 response in a murine model of pancreatic cancer liver metastasis[J]. J Immunother Cancer, 2020, 8(2): e001367.
[23] Jang JY, Kang MJ, Heo JS, et al. A prospective randomized controlled study comparing outcomes of standard resection and extended resection, including dissection of the nerve plexus and various lymph nodes, in patients with pancreatic head cancer[J]. Ann Surg, 2014, 259(4): 656-664.
[24] El-Hadaad HA, Wahba HA. Oxaliplatin plus 5-fluorouracil and folinic acid(OFF)in gemcitabine-pretreated advanced pancreatic cancer: a phase Ⅱ study[J]. J Gastrointest Cancer, 2013, 44(3): 313-317.
[25] Peng R, Zhang PF, Zhang C, et al. Elevated TRIM44 promotes intrahepatic cholangiocarcinoma progression by inducing cell EMT via MAPK signaling[J]. Cancer Med, 2018, 7(3): 796-808.
-




 下载:
下载: